Women are more likely to experience tooth decay, inflammation and bleeding gums in pregnancy. This can trigger premature births and harm the development of newborns, but you can lower these risks by looking after your dental health while expecting a child.
—
Expect to lose a tooth for every baby you bring into the world.
Have you ever heard this old wives tale?
Thankfully, it’s not true – pregnant women can keep all of their teeth, by being diligent about their oral health.
But this takes more effort than usual…
The combination of sugar cravings, hormones and vomiting leads to gum inflammation (or gingivitis) in up to 70 per cent of expectant mothers.
We see more women with bleeding gums during pregnancy at Mona Vale Dental. This is usually temporary, but can turn into a severe form of periodontal gum disease, if untreated.
Alarmingly:
Periodontitis can harm unborn babies and lead to premature births, some research suggests.
Doctors even linked gum disease to a documented case of a stillbirth in the USA. If more people were aware of the potential risks, they’d go out of their way to protect their teeth.
Unfortunately, this isn’t the case.
Most women avoid seeing the dentist when they’re pregnant because they believe it’s unsafe. This needs to change. You could seriously damage your teeth by failing to take extra precautions during pregnancy.
And if the research is correct, this could even harm your developing baby.
Nobody intends for this to happen, but we must address this risk.
Premature birth is linked to poor oral health (research)
Around one million children die from problems that arise from preterm births every year, according to the World Health Organisation.
Can a tooth infection harm my unborn baby?
Yes, we’re now learning that bad oral health while expecting could heighten these risks:
- Preterm birth
- Low birth weight
- Preeclampsia
- Gestational diabetes
- Chronic lung disease
- Breathing difficulties
- Jaundice
- Problems with temperature control
- Feeding issues

What the experts say:
Some research suggests that periodontal disease triggers 18 out of 100 premature births.
Another study in the UK didn’t reach this conclusion, but found a link between gum disease and miscarriage.
Now, it’s worth noting the jury is still out about all of this.
There have been limited studies (especially in the developing world), and the results are contradictory.
Charlene Africa is a Professor of Medical Biosciences at the University of the Western Cape.
We should be worried, if her investigation in Africa is anything to go by.
Her team found a connection between underweight preterm babies and mothers with periodontal disease. These women lacked adequate proteins that reduce infection in the body.
When this happens, the body can go into early labour.
Our studies confirmed that when a woman had periodontal disease there was an imbalance in these proteins which could create an inflammation in the woman’s body and induce preterm labour.
Professor Charlene Africa, The Conversation
On the other hand, researchers found that women without gum disease were more likely to have normal pregnancies.
For those with periodontitis, an early diagnosis can lower your chances of having a premature delivery, according to Professor Africa.
Unfortunately, not enough people know this.
The challenge is that not many mothers seek dental treatment for bleeding gums during pregnancy. And antenatal clinics pay little, if any, attention to the mother’s oral health status. As a result, this complication often goes undetected.
Thankfully, a little awareness can go a long way towards supporting a healthy, full-term pregnancy.

Why do problems emerge with pregnancy and gum disease?
- A flood of hormones
- Sugar cravings
- Too much vomiting erodes enamel
Women produce more hormones when expecting – particularly oestrogen and progesterone.
This sudden and dramatic surge helps the uterus and placenta to transfer vital nutrients to unborn babies.
Such changes are essential, but can wreak havoc on your oral cavity, if you’re not careful.
Many women notice bleeding gums in pregnancy, when brushing or flossing around the two-month mark.
This is because tissues and ligaments soften to prepare for labour. There’s more blood pumping through your veins and gums become sensitive to bacteria in plaque.
And the timing couldn’t be worse, especially if you’re craving chocolate 24/7!
Spare a thought for the countless women who spend their mornings heaving up the contents of their stomachs too.
The acid from vomit can wreak havoc on enamel, especially if you’re suffering from hyperemesis gravidarum (a serious pregnancy condition that turns the simple act of brushing your teeth into a nightmare – more on this later).
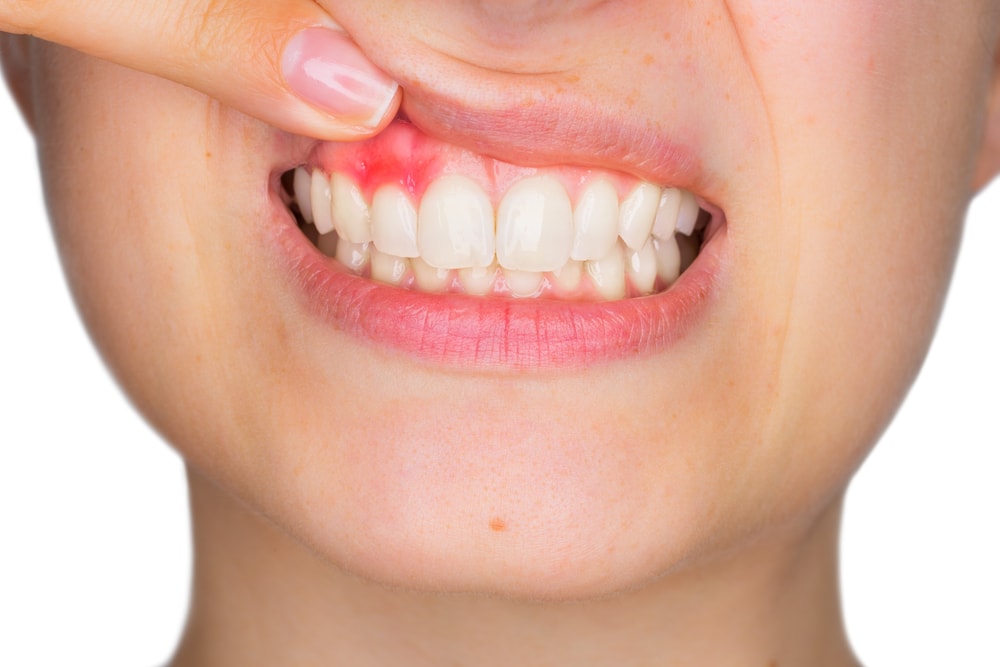
Common dental problems when expecting
Bleeding gums in pregnancy (gingivitis):
Is it normal to have bleeding gums during pregnancy?
Yes, but please don’t ignore it.
Nearly half of all pregnant women experience swelling, bleeding or redness when they brush or floss their teeth. This happens when bacteria builds up, causing gum inflammation.
Generally speaking, women who’ve maintained their oral hygiene won’t be affected.
How to get rid of pregnancy gingivitis:
If you develop this condition, it can be easily managed by a dentist, as long as you get there in time. Thankfully there’s no irreversible damage to bones or tissues in the early stages.

Although this condition is often temporary, it can weaken the tissues that support teeth.
The real concern is:
Left untreated, mild gum inflammation turns into periodontal disease, which can be serious – for both mother and baby.
Periodontal gum disease is more concerning…
Periodontitis is gum disease at its very worst – it emerges when tissues surrounding the teeth become infected after gingivitis. Small spaces form between the teeth and gums, trapping debris and spreading bacteria below the gum line.
As a result, the gum tissue and bones deteriorate and no longer hold teeth in place.
Keep in mind:
This is the leading cause of tooth loss in adults, and it’s linked to premature births in some studies.
Signs and symptoms of periodontitis include:
- Inflamed or swollen gums
- Small pockets surrounding teeth (2-3 mm)
- Constant bad breath
- Loose teeth
- Tenderness or pain when biting or chewing
- Tooth loss
- Sore, bleeding gums
- Bad taste
- Receding gums, making teeth look longer
- Thick, yellow fluid or pus on gums
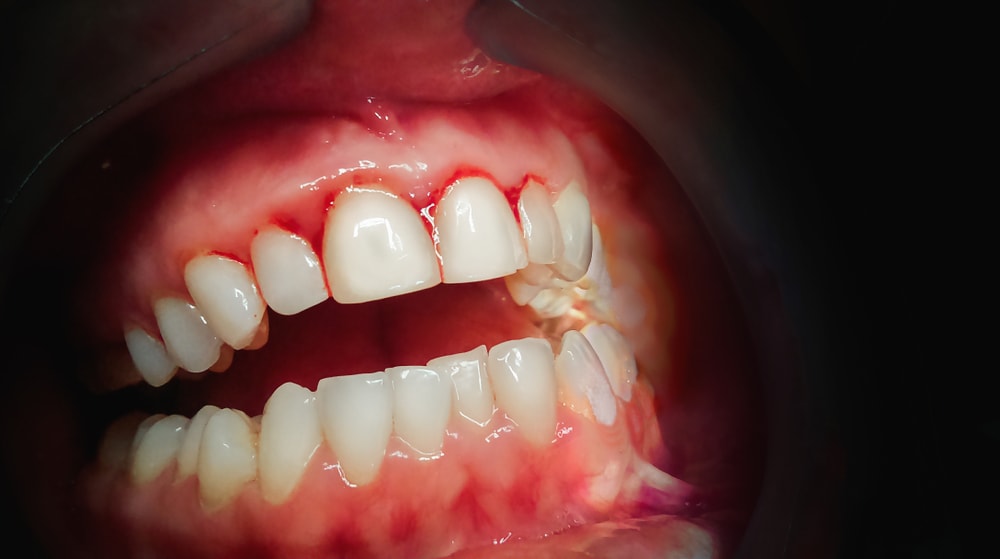
Can anything be done about swollen, red and bleeding gums in pregnancy?
Thankfully, yes.
How to treat gum disease:
In mild cases, dentists can reverse gingivitis by controlling the amount of bacteria in your mouth. This involves professional deep-cleaning and mouth rinses to remove hardened plaque.
In more serious scenarios, antibiotics are prescribed and dental surgery may be required.
The good news?
Treatment for periodontitis is usually successful, if the condition is detected early enough.
But as always, prevention is best. Correct brushing techniques help to minimise bleeding and stop inflammation from spreading. Keep reading, we explore this in more detail later on.
Pyogenic granuloma (pregnancy tumours)
If you happen to notice red lumpy lesions along your gum line and between teeth, don’t panic.
This is fairly common, affecting one to five per cent of pregnant women globally, usually during their second trimester.
The lesions should disappear after birth, since elevated hormones are to blame.
What do they look like?

It’s important not to pick, scratch or remove the lesions yourself, as this makes it worse.
You might have a single tumour or multiple nodules. These are benign (non-cancerous) and tend to be located on the mouth or skin.
Your dentist will diagnose the condition with an examination, to eliminate other disorders. They can remove the lesion, if it makes chewing or swallowing difficult or causes pain.
Otherwise, it’s best to wait and see if the growth shrinks (along with your baby bump) after delivery.
Tooth decay in pregnancy
Err on the side of caution and visit your dentist, if you get a toothache during pregnancy.
It could be a red flag that bacteria is damaging enamel. This happens when food particles mix with acids and saliva to form plaque that lingers on your teeth.
Cavities often emerge during pregnancy, especially if you’re chowing down sweet foods to satisfy intense cravings.
Signs and symptoms of tooth decay:
- Oral pain or increased pressure
- Sensitive teeth and tenderness when eating and drinking cold or hot foods and drinks
- Bad breath
- A hole or pit in the tooth
- Brown, yellow or grey spots on your teeth
- A foul taste in your mouth
- Pus around the tooth
A strong oral hygiene routine helps to keep decay at bay during this time. Unfortunately, this is very difficult for women with hyperemesis gravidarum.

Hyperemesis gravidarum during pregnancy
“Over the past 14 days I’d vomited at least 20 times before midday (impressive when I could barely eat or drink), peed in a cup my husband held underneath me because I couldn’t physically get out of bed, not showered nor brushed my teeth because I didn’t have the strength to even lift my arm and lost 3 kilos, along with my dignity.”
Katherine Pinner
Most women experience some degree of nausea and vomiting. Pregnancy is tough on the body, even at the best of times.
Throw a medical condition called hyperemesis gravidarum into the mix and it becomes unbearable for 2 per cent of expectant mothers.
And in many cases, dangerous! Around 1000 women a year terminate their pregnancies because their bodies can no longer sustain it.
The complications of HG include:
- Excessive vomiting, at least a few times a day
- Persistent nausea
- Dehydration (resulting in hospitalisation)
- Electrolyte imbalance
- Rapid heartbeat
- Headaches
- Confusion
- Depression
- Weight loss
- Fainting
- Chronic fatigue

Severe vomiting can ruin your teeth
“Sometimes it’s downright impossible for women with HG to brush their teeth. Even me, a dental hygienist, went at least a month at one point in one of my pregnancies without brushing my teeth. That’s a dental sin if I’ve ever heard of one.”
Sharon Boyd, a dental hygienist who had hyperemesis
Women at the extreme end of HG might vomit more than 30 times a day.
To add insult to injury:
The simple act of using a toothbrush or mouthwash can cause gagging, making cleaning impossible.
It’s not uncommon for these expectant mothers to go for weeks (even months) without brushing their teeth.
Can you imagine what this does to oral health?
Gastric acid from frequent vomiting erodes tooth enamel and heightens the risk of tooth decay and gum disease.
Long-term consequences of HG include:
- Tooth loss
- Multiple fillings
- Root canals
- Pain and sensitivity
- Discoloured teeth
- White spots
- Weak and crumbling teeth
Women with hyperemesis gravidarum often struggle to hold down food and have no appetite. Sugary snacks seem to be easier to stomach, leading to frequent consumption.
Talk about a double whammy!
Poor oral hygiene + excess sugar = an environment where decay thrives.
“I’ve had nothing but dental problems after my 2 HG pregnancies. Severe vomiting and nausea, made me unable to brush my teeth for great periods of time. Putting a toothbrush into my mouth would make me gag. The acid from vomit erodes tooth enamel, leaving your teeth weaker and more susceptible to problems. Because I didn’t brush my teeth while I was sick, I also suffered severe plaque build up on my teeth which really seemed to push my gums down. Now all my roots are exposed and I have very sensitive teeth.”
Comment on hyperemesis forum
It’s important to seek help if you have HG, before the decay sets in. Your dentist can suggest gentle ways to keep your mouth clean. We explore some of these solutions below.

How to protect your oral health in pregnancy
Wait an hour after vomiting to brush your teeth
Your teeth are covered in acids from your stomach after vomiting, which softens enamel. The last thing you want is to brush vigorously and scratch that enamel away – exposing teeth to decay.
Instead, rinse your mouth straight away. You can also add a teaspoon of baking soda to warm water, which helps to neutralise the acid.
Is retching a problem when you clean your mouth?
- Try a soft toothbrush with a smaller head, or a toothbrush for toddlers. Brush slowly and listen to music, if you need something to distract you from the gagging reflex.
- Brush the back of your teeth before cleaning the rest of your mouth. This allows you to avoid the taste buds on your tongue for as long as possible.
- Experiment with different toothpaste brands until you find one that doesn’t make you gag. Ask your dentist if they have any free samples you can try.
- Sensitive toothpaste is an excellent option for women who gag while brushing. The fluoride is still there, but the flavour isn’t strong and there are no foaming agents.
- Consider carrying a small toothbrush and toothpaste with you, when you’re out. You might struggle to brush first thing in the morning, when nausea is bad, but maybe you won’t have the same gagging reaction a little later in the day?
- As a last resort, try brushing without toothpaste, if the very thought of it makes you sick. Alternatively, put the tiniest amount on your finger and rub this over your teeth, before rinsing.
Make sure your toothpaste contains fluoride
Adequate levels should sit between 1000 to 1500 ppm. Your dentist will tell you if you need a high concentration product (prescription).
Use a fluoridated mouthwash, if you can tolerate it
Choose a brand that has a mild flavour, so it’s easier to swish in your mouth.
Eat well and limit sugary foods
We know this is easier said than done, especially when intense cravings take over! Sometimes fresh fruit with Greek yoghurt is enough to hit that sweet spot.
Acid-neutralising foods like milk and hard cheese work well too.
It’s also important to get plenty of calcium and vitamin D in your diet (good sources include yoghurt, cooked fatty fish and fully cooked, pasteurised eggs).
Drink sugary beverages through a straw!
This minimises the amount of acid that touches your teeth.
Chew sugar-free gum that contains xylitol, especially after sugary snacks.
This creates more saliva, which neutralises some of the acid in your mouth. Women with HG tend to complain about a lot of saliva, but this can actually work in your favour.
Dental work when pregnant – what treatments are safe?
We strongly recommend getting regular cleanings and checkups.
Make sure you always tell your dentist that you’re pregnant. He or she will tell you what medications and procedures are safe, during different stages.
It’s best to postpone elective procedures until after delivery. But if you can’t wait, the second trimester and start of the third trimester are the most suitable periods.
If possible, avoid getting a treatment during your first trimester. This is when the baby develops organs and is particularly vulnerable to chemicals.

Can you have a dental x-ray when pregnant?
Avoid x-rays where possible, unless it’s an emergency.
Your dentist will take precautions to protect your baby, such as using a lead apron and thyroid guard, as well as minimising your exposure. Dental x-rays with lead shielding are safe, according to the American College of Radiology.
These days, dental x-rays emit very low doses of radiation, so there shouldn’t be negative effects from one scan.
Dental fillings during pregnancy
The second trimester is the best time to get cavity fillings or crowns, if you need these to fight infection.
Having said this, you might need urgent treatment during your first or third trimester, if you’re in a lot of pain. Your dentist will tailor their approach to make sure you’re comfortable and safe.
Local anaesthetic in pregnancy
Is dental anesthesia safe during pregnancy?
Yes, as long as suitable anaesthetics are used. Any containing felypressin, for example, should be avoided, if possible, since it constricts the blood vessels. This can cause some contractions in the uterus.
It’s unlikely that such low levels will do this, but it’s best to err on the side of caution. Be sure to tell your dentist that you’re expecting. They will choose the safest option and dosage, depending on how far along you are.
Again, elective surgeries can wait until after the birth.
Is teeth whitening safe during pregnancy?
The risks are minimal but it’s best to wait until after you’ve stopped breastfeeding, since this isn’t an urgent procedure.

Safe painkillers in pregnancy
Do you have a toothache that doesn’t go away?
Swelling in your mouth?
A dislodged filling?
Dental emergencies often occur at the worst times, when we can’t get help straight away. Ideally you’ll visit your dentist on the same day, however this isn’t always possible.
In these cases, it’s important to manage your acute pain, until you can get to a clinic.
This can be tricky when you’re expecting, since certain medications come with risks to the baby.
What about non-prescription or over-the-counter drugs for pain management?
Always ask your doctor or pharmacist first, to be certain you’re choosing a safe option.
Many expectant mothers, for example, take paracetamol, which is relatively safe. However, it should only be used when necessary and only for a short time.
Health Direct, a national government organisation, advises that pregnant women avoid taking non-steroidal anti-inflammatory drugs like ibuprofen, nurofen and aspirin.
These have been linked to complications and could heighten the risk of miscarriage.
It’s also best to avoid opioid painkillers during pregnancy, since these can harm your unborn baby. But speak to your doctor before stopping any prescription medicines that you’re already taking, as this might have unintended consequences.
What can you do if you don’t feel comfortable taking any oral medication?
Benzocaine is an over-the-counter antiseptic that provides some degree of pain relief as it numbs the gums. You can smear it over the irritated teeth or gums. This is generally considered safe as a short-term fix. As always, you should exercise caution and check with your doctor. Keep in mind there are limited studies into the safety of this compound.
And if you want to avoid chemicals completely?
Some women choose not to take any medication while expecting. If this is you, there are a handful of natural solutions that might provide some relief until you can see your dentist.
(click image to enlarge on desktop)
The Health Direct hotline (national) is open 24 hours, 7 days a week: 1800 022 222
MotherSafe in NSW: 1800 647 848
ACT Alcohol and other drug service: (02) 6207 9977
Royal Women’s Hospital in Victoria: (03) 8345 3190
Women and Children’s Hospital in South Australia: (08) 8161 7222
Obstetric Medicines Information Service in Western Australia: (08) 6458 2723
Northern Territory Drug Information Centre: (08) 8922 8424

Cavities are contagious (another reason to protect your teeth)
So far, we’ve focused on the dangers that a mother’s dental problems pose to her unborn baby.
But there’s another reason why pregnant women (and all adults) must look after their oral health.
Cavities are contagious, like an infection.
This means you can pass on tooth decay (dental caries) to your young children, if you’re not careful.
“Alarmingly, one in four Australian children aged 5–10 have tooth decay that is not being treated.”
Cancer Council Victoria
Do you ever share a spoon with your toddler or clean their dummy by putting it in your mouth?
This seems harmless enough, but it isn’t.
You could be spreading caries-producing bacteria to babies, toddlers and young children.
Many people are completely in the dark about this!
This is shocking, considering tooth decay is the leading chronic disease for children. It causes pain and embarrassment, as well as making eating and swallowing difficult.
Even worse:
Tooth decay might worsen existing health conditions. It also increases the risk of developing heart disease and other chronic illnesses.
Nobody wants this for their child.

This means no:
- Kissing on the mouth
- Sharing utensils or toothbrushes
- Holding a dummy in your mouth or cleaning it with saliva
- Sharing food or drink
- Blowing on your baby’s food to cool it down
- Letting babies or toddlers put their fingers in your mouth
You should also visit your dentist and maintain good oral hygiene, during and after pregnancy.
Read more about tooth decay in children here.
Bleeding gums in pregnancy or other problems? We can help …
Mona Vale Dental is committed to providing the best dental care for pregnant patients.
It’s important that you feel comfortable, relaxed and safe, every step of the way.
We also specialise in children’s dentistry, for when your little one is ready for their first check-up.
Please contact us on (02) 9997 1100 to book an appointment or find out more.




